The healthcare industry is accustomed to innovation. Interoperability, data analytics, precision medicine -- technologies that innovate and maintain the quality of care are being celebrated every day. They are all great, but what do you do when a patient simply doesn’t follow up with a visit? How can you help when people fail to take their medication? And how can you be sure that they are willing to go the proposed treatment route when they don’t seem to fully understand the risks and consequences?
Even the most inventive therapy and highly acclaimed doctors don’t work in a vacuum. A patient’s behavior and even beliefs affect the outcome just as much as what the doctor does. So, how do healthcare providers motivate patients to take an active part in their healthcare?
Why you need patient engagement software
Patient engagement covers tools or strategies that help patients actively participate in their own healthcare. Either due to low health literacy or the current design of care delivery, a typical patient is rather passively involved in managing their own care.
Take Joan, a 63-year-old patient with glaucoma. She’s losing vision in one eye and high pressure in the other eye may result in her becoming blind in both eyes. Her doctor gives her two options: removing the eye with lower visual activity to help manage the pressure in the other eye and preserve vision, or try to slow down the vision deterioration with medication.
Joan has to consider a lot to make a decision: the trauma of the possible loss of an eye, the cost of medication and the surgery, the risks both options have. Not understanding many nuances of her own conditions, she has to rely on the support of her family and doctor to make this choice for her and to make sure she recovers well. Even if her family makes the best choice for her, it may not serve her confidence in the future when she’ll have to self-manage her health on a daily basis on her own. This level of knowledge, skills, and confidence -- or, in short, engagement -- is a crucial part of improving health outcomes.
High patient engagement is based on a combination of three core practices:
- education - explaining their condition and course of the treatment to patients,
- decision making - involving patients in selecting their treatment,
- support outside the office - providing tools to help patients adhere to a treatment plan.
A handy representation of patient engagement is the Patient Activation Measure or PAM -- a survey assessing patients on one of four levels.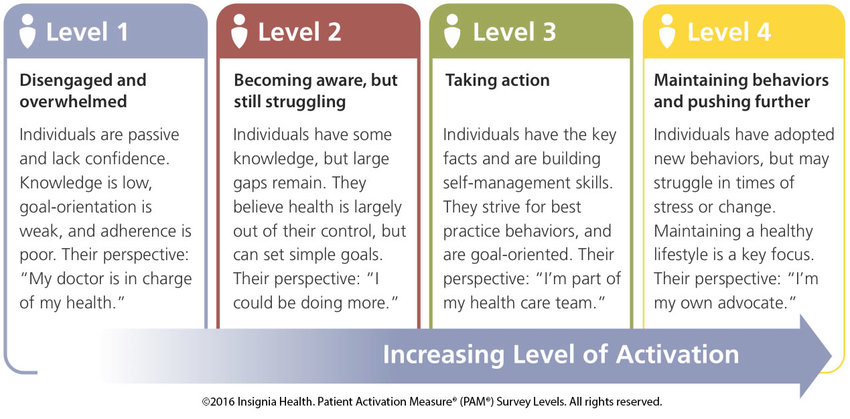
Level 1 - People who don’t understand their role in managing their own health, act passively, and rely on doctors to tell them what to do.
Level 2 - People with knowledge gaps but are able to stick to simple routines.
Level 3 - People who know how to take care of their health but lack some knowledge or skills.
Level 4 - People who adhere to many routines and behaviors to support their health, capable of maintaining this lifestyle independently.
Patients like Joan who are estimated to be from 25 to 40 percent of the population are stuck on the first and second levels. To improve their confidence, understanding, and help them build good habits, healthcare providers use different tools and techniques.
Patients on levels 3 and 4 don’t need that much attention but can be helped by the same tools and methods to help them manage their condition better.
Now, what software functions can help you achieve high patient engagement in your practice? Here are some options.
Implement a patient education platform
Patients with low health literacy are also less likely to look into educational materials. So, it’s your responsibility to give them that information. The time you spend interacting with patients, your communication style, and the mode of information provided are all important in teaching patients about their conditions. Unfortunately, doctors usually don’t have the time and energy to communicate this knowledge. Traditional brochures, charts, PowerPoint presentations, physical models, videos, and podcasts are great, but it’s difficult to curate a collection of evidence-based information for each patient.
And that’s why you should use an educational platform.
A patient education platform is a suite of tools that permits healthcare workers to deliver high quality educational materials to patients. Unlike usual handouts, interactive digital content can be easily customized, shared, and augmented with additional functions, like dashboards and multiple language options.
Components
Support for clinical codes and standards. Healthcare standards are the backbone of effective data management. You can use them for easy search and filtering in the database, or link content between different parts of the system, for example, when leaving instructions for patients in an EHR or on the Patient Portal.
Ability to create and upload custom content. Patient education materials are usually written by dedicated companies, and software providers partner with them to use this information and present it in an interactive manner. But it’s likely that your clinic would want to upload your own images, presentations, or videos. The platform should have a toolset for content management. Elsevier, for example, serves as a central hub for all your proprietary content, making it accessible both via EHR and its education platform.
Content at different levels of comprehension. It’s reported that the average Medicare beneficiary reads at a fifth-grade level. So, for optimal comprehension, patient education materials should be written at a sixth-grade or lower reading level. For multilingual populations, it makes sense to provide education in a few languages. For example, AdvancedMD has materials both in English and Spanish.
Dashboard and reporting. Data gives a meaning to every action. Here, it gives hospital staff an outlook at each patient’s progress, needs, and satisfaction. The SonifiHealth platform has tons of analytics regarding how patients interact with educational materials: what content they’ve viewed and what types they preferred. There, you can also track engagement scores like PAM allowing you to pay more attention to patients who have the highest risk of complications post-discharge.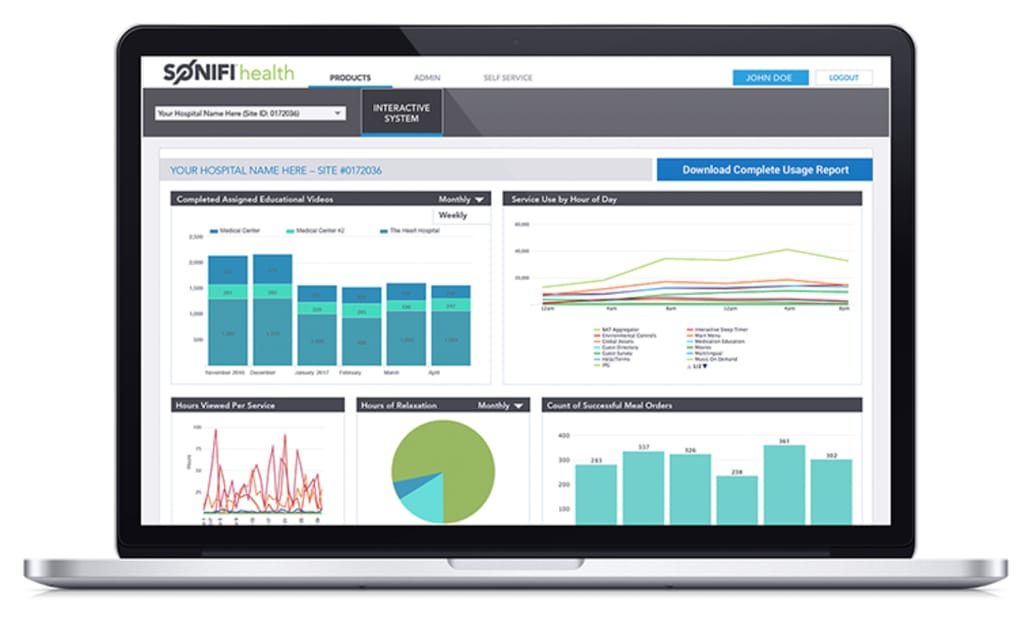
Automatic analytics also engage staff, giving them more information without additional workload
Implementation
Patient education software can be implemented in two ways.
Web-based platform. A library of instructional text, images, and videos, where caregivers choose among peer-reviewed, trusted materials, document them in an EHR, and make them accessible to patients on the hospital’s website or patient portal. They are easy to use and develop custom.
Combination of hardware and software. Depending on the vendor, these are TV screens and controllers installed directly in a clinic. They are meant to relieve the stress for recovering patients, address concerns of people waiting in the lobby, and help ease the load off healthcare workers by answering some of the most common questions. Although there are many out-of-the-box options, with a skilled technology team, the custom route is possible too.
Introduce decision aids for shared decision making
Shared decision making that involves both a doctor and a patient has a lot of significant benefits. When patients take part in deciding what treatment plan to use, they have less anxiety about procedures and are less likely to receive unnecessary treatment.
Decision aids are resources and tools that help patients and doctors discuss different treatment methods. (Don’t confuse them with Clinical Decision Support Systems helping medical professionals in their decisions.) Decision aids come in all forms -- videos, web-based tools, apps, clinical calculators, and more. The example below is a decision aid developed by the Mayo Clinic to help patients choose an antidepressant by reviewing the side effects of common drugs.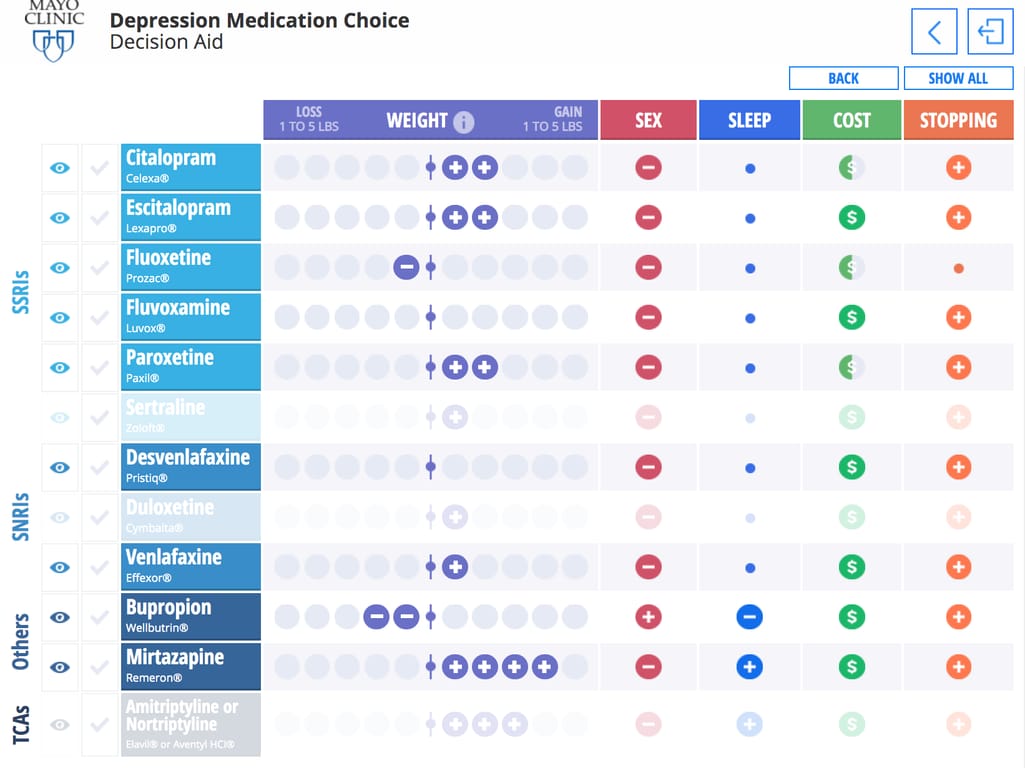
This depression medication comparison gives an idea of how the drug will fit into a patient’s everyday life, not their effectiveness in the treatment Source: Mayo Clinic
There are different options for decision aids implementation. You can always go with text and videos, but there are some more interactive options.
Components and types
Active learning resources. Active learning is not inherently different from passive resources such as articles and brochures, but its interactive nature promotes more attention from patients and allows you to include different media formats. For example, in a decision aid for driving with dementia, you must click on the screen to reveal the parts of text. It also includes videos with stories from people with dementia. Patients may also reflect on some parts of the information and write down their thoughts in a notebook.
Options comparisons. Prominent decision aids provider Healthwise uses a course-like structure. First, the patient gets the overview of their options (to get or not get allergy shots) and some vital information. Then, options are compared by different parameters, such as benefits and side effects. In the third section, a patient can express their feelings for different reasons to take or not take the shot. For example, if they can avoid allergens, it may be a strong enough reason to not take a shot. Then, they can point out their decision and their certainty. Finally, there’s a quiz to check how well a patient understood all provided information and a summary of the decision.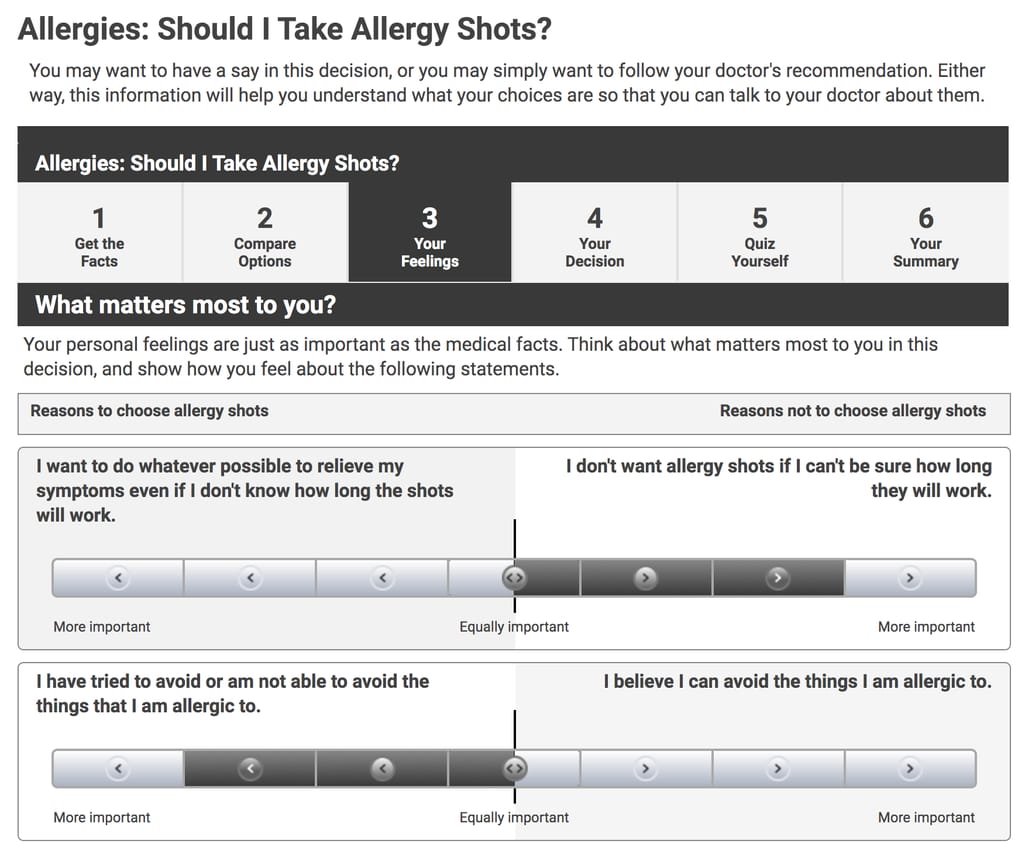
Such decision aids help patients not only consider the facts but also their thoughts about medications and procedures Source: Healthwise
Implementation
While paper and video-based decision aids can be shared by different means such as email or by a link, interactive aids should be integrated into your system via APIs. Popular developers like Healthwise provide these connectivity options to merge their content with your EHR and patient portal, so you can control how patients access and progress through decision aids, and, of course, include custom notes. Make sure you have a team of tech professionals to support this integration.
Adopt secure messaging, scheduling, and outreach
In the US, the lack of medical adherence is estimated to cause around 125,000 deaths and 10 percent of hospitalizations. Changing someone’s behavior requires more continuous effort and checking-in, and one of the most effective solutions is messaging. Automated communication reminds patients when it’s time to take, order, or pick up their prescription refills. This is part of the telehealth technologies that are quickly becoming the norm in modern healthcare.
Patient-doctor communication technologies are different types of chats, video calls, auto messaging, and reminders that streamline patient follow-up and improve engagement. A secure, HIPAA-compliant communication channel makes it easier to send education materials, lab results, and insurance cards. It’s also mobile-friendly and can reach more patients than via the patient portal.
Components
Medicine adherence reminders. There are many reasons why someone may not adhere to taking their meds. People may not experience any symptoms and might feel that they don’t need medication anymore. Some people are reluctant to become dependent on meds in their daily lives. Patients with mental illnesses simply may not have the motivation to continue with the treatment. A reminder set up during a doctor visit can make sure that a patient takes a drug correctly, at the right frequency and length of time.
Appointment reminders and scheduling. Automated appointments and follow-ups can be programmed to activate less engaged patients, all without increasing the volume of work for physicians.
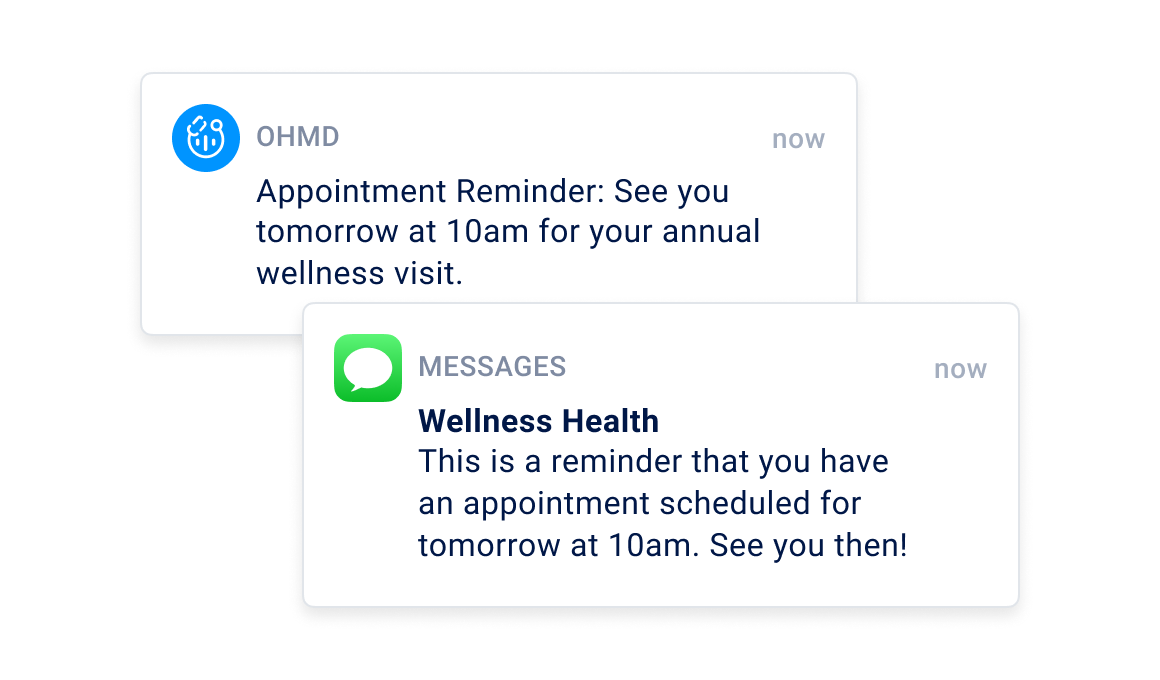 Scheduling reminders eliminate no-shows and are more effective than emails or phone calls Source: OhMD
Scheduling reminders eliminate no-shows and are more effective than emails or phone calls Source: OhMD
Procedure updates. Texts can also be used to update family on the progress of the procedure or send automated information on surgery milestones as done by MyCareText.
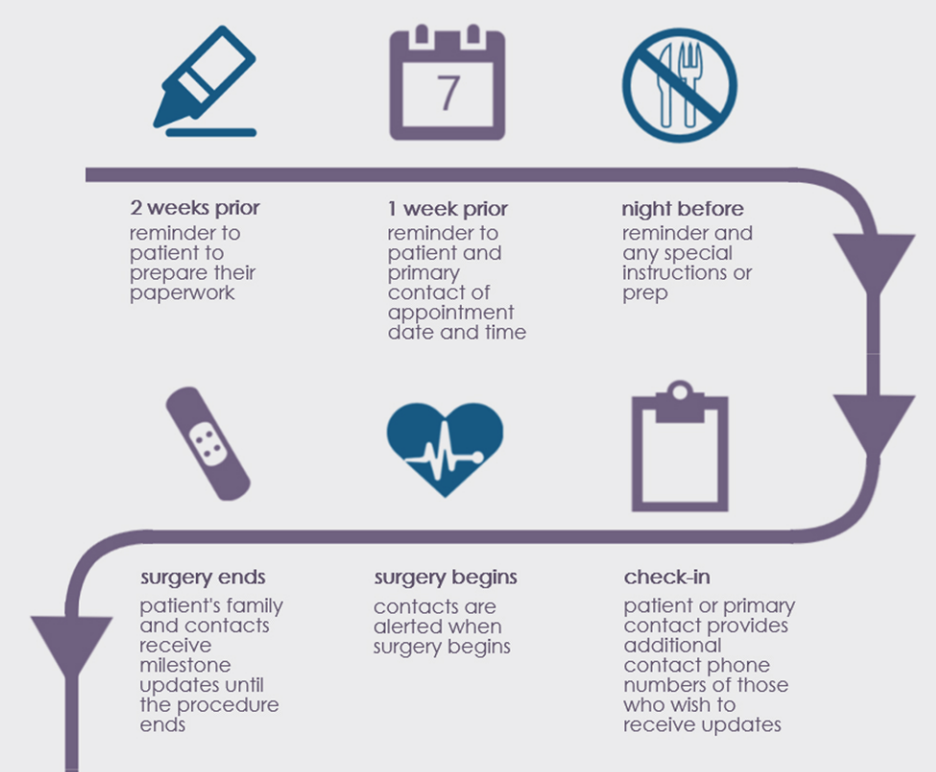
Examples of messengers a patient or family can receive during prior and during the procedure Source: MyCareText
Implementation
Each type of communication, whether it’s live SMS texting, web chat on the portal, or appointment reminders can require different integration options. These are the most popular and accessible ones.
SMS. Here, a patient doesn’t need to download any apps, but you access your messaging history via an EHR. Besides, the same technology can be used for staff communication. But there are considerations about HIPAA, as the rules don’t specify if patient data can be sent via SMS. If you want to remain on the safe side, use this approach only when sending messages that don’t contain personal information.
Texting apps. Apps like WhatsApp and Telegram provide APIs for connecting with your internal systems. They often allow you to create secret chats that provide an additional level of encryption, have convenient media sharing features, and if you know how to work with APIs, you can configure them to your liking.
Now, what’s the process of introducing these processes and tools in your practice?
How to adopt patient engagement strategies and solutions
Step 1. Start calculating the engagement level of your patients
Understanding the engagement level of each patient helps providers be more realistic about the next steps in care. Heavily engaged patients can be expected to do their research on the conditions, apply medication routines, and even change their eating habits, while patients with lower confidence need access to education and more nuanced recommendations.
These are the three main scores that will help you understand the engagement situation at your facility:
- CAHPS (Consumer Assessment of Healthcare Processes and Services) that surveys patient satisfaction and experience,
- PAM (Patient Activation Measure) that calculates the engagement level of each patient,
- PROM (Patient-reported Outcomes Measure) that studies the positive or negative effect of provided care.
Collect this data to review the overall success of your clinic and reveal your most problematic areas. After seeing what needs improvement, prepare for technology solution adoption.
Step 2. Assess your technology options
You can take one of the two ways to integrate patient engagement functionality in your practice.
Patient portals. The most accessible implementation method of these strategies are via patient portals. Also called electronic personal health record or ePHR, this software is ideally linked (tethered) to a hospital’s EHR and allows patients to access and manage their health information such as laboratory results and medication lists. In some instances, patients can even request prescription refills, make payments, or message with a doctor. Epic, Cerner, Greenway, eClinicalWorks are EHR providers with integrated patient portals.
Patient engagement solutions. Providing more flexibility and coming at a lower price, these tools are targeted at covering your specific engagement goals. Education platforms, telehealth solutions, messaging, and scheduling systems are often provided in the cloud.
Check with your provider what patient portal options they offer and their implementation methods. If you don’t find the ones you’re looking for, custom development would be your best option.
Custom patient engagement system. Considering the complexity and security issues that come from healthcare software integration, your best option might be doing it yourself. Besides, creating a custom solution will help overcome many implementation barriers engagement software has, like poor UX that your staff and patients will have to come to terms with, or the disparity between out-of-the-box software and your internal processes. Of course, to do that, you’d need a product development team.
Step 3. Select or employ a development team
If your EHR vendor doesn’t offer IT support or you’re going down the custom road, you’ll need technology staff. These are some of the crucial roles.
Product manager. Your IT lead, CTO, or CIO may perform a product manager role by defining your needs, choosing a tech stack, and creating an implementation plan. But if you don’t have such a specialist, prepare to find one that has managerial, usability, and tech skills along with knowledge of the healthcare domain.
UX designer. If you want staff and patients to actually use an engagement system, make sure to work with a UX professional. Bad usability in EHRs is one of the biggest, most frequent problems physicians face daily, so make sure to not add to the burden.
HIPAA compliance specialist. Healthcare solutions come with security challenges and must adhere to HIPAA privacy rules. Cloud or on-premise, data centers should use high-level security and regularly conduct risk assessments. Remember that messages should be encrypted. If you don’t have a HIPAA compliance officer, you will need one.
Patient engagement adoption obstacles
The success of patient engagement strategies and technologies is well documented but critically underused. There are challenges to integrating them in the care process and accessing by some patients.
Bad user experience. Patient portals can be clunky to use. Even when information is offered, it’s often hard to find or review. And well-meaning notifications about upcoming appointments or handy educational materials become annoying.
Technology gap. Elderly populations may find it hard to rely on the internet or email, so they require extra attention or the help of families to navigate digital spaces. When clinics don’t have strategies for incorporating tech into elder care, everyone loses -- providers can’t automate operations and patients don’t receive the benefits.
Pushback from health providers. Doctors often don’t believe that they need help in communicating with their patients. So, IT leads of the hospitals should “sell” the technology to doctors as well. When they do that successfully, physicians will start promoting the tools to the patients.

Maryna is a passionate writer with a talent for simplifying complex topics for readers of all backgrounds. With 7 years of experience writing about travel technology, she is well-versed in the field. Outside of her professional writing, she enjoys reading, video games, and fashion.
Want to write an article for our blog? Read our requirements and guidelines to become a contributor.