An average adult makes about 35,000 decisions daily. The majority of them are trivial choices about clothing, food, or other things that — no offense! — don’t really matter. But everything changes as we enter the healthcare field where the right decisions save lives while the wrong ones lead to grave consequences.
To pinpoint the best solution for a particular patient or case, health workers have to sift through numerous details and factors — and do it fast, under a great deal of pressure. Luckily, the most routine part of this job can be done by computers — or, to be more specific, by clinical decision support systems. This article explores how these technologies can improve the speed and quality of medical decisions.
CDSS basics: types, tasks, and structure
Broadly speaking, a clinical decision support system (CDSS) is a program module that helps medical professionals make decisions at the point of care. The concept is not new to the healthcare sector: The first CDSS called MYCIN was built in the early 1970s at Stanford University. It employed an artificial intelligence model applying over 600 rules to identify infectious diseases and recommend a course of treatment.
Though MYCIN outperformed medical staff in evaluation accuracy, it was never put in practice — partially, because of slow performance, but mainly due to the ethical and legal issues. The very idea of the computer acting as a medical expert was too ahead of its time to be accepted.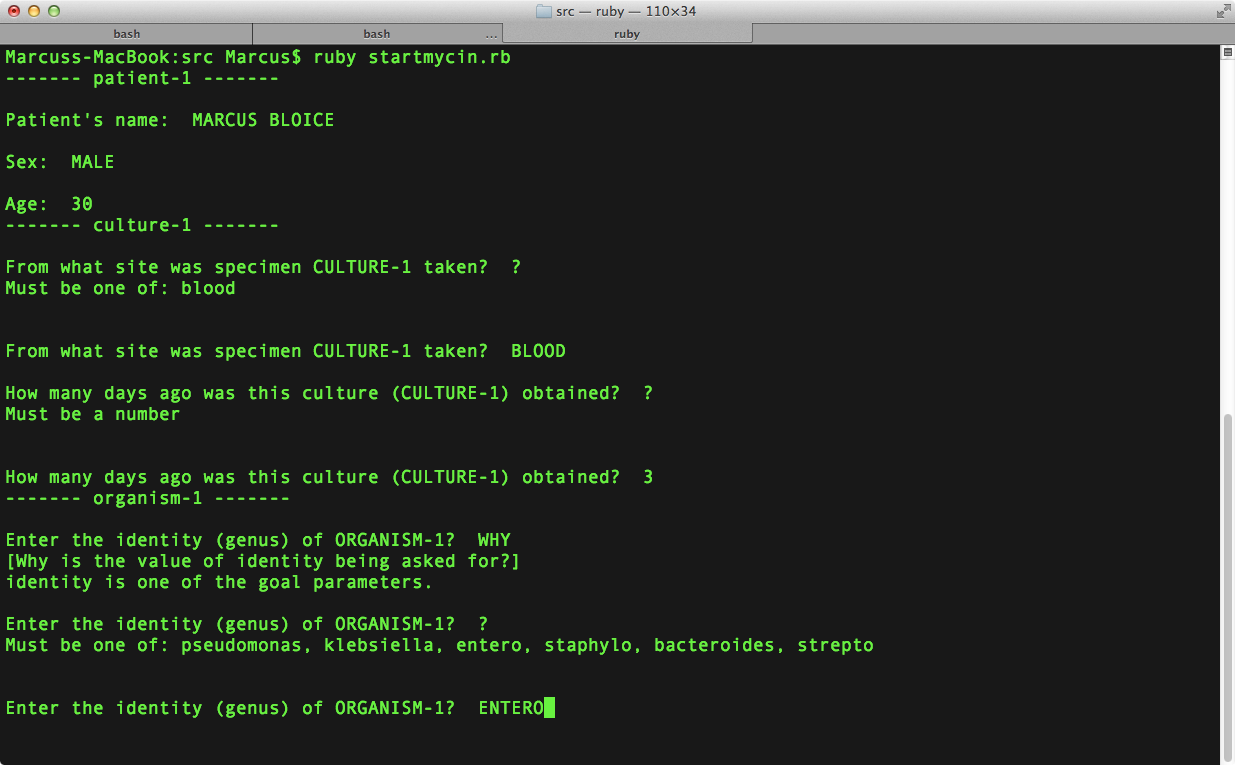
MYCIN expert system interface
Now, hospitals use CDSSs for numerous tasks, from generating alerts to drug control to ordering tests. Decision support solutions come in a number of versions. They can be either standalone tools or integrated parts of larger infrastructures — such as an Electronic Health Record (EHR) or a Computerized Provider Order Entry (CPOE) system, designed to replace a paper-based ordering process. Some of them focus on a single problem and perform simple functions — like sending reminders. Others cover a wide range of processes and include multiple modules.
No matter the size, modern systems benefit from powerful computing engines, cloud technologies, and advanced algorithms. But at the architectural level, they haven’t changed much over the last decades, preserving structures similar to early expert solutions.
CDSS architecture
A typical CDSS contains three core elements: a base or data management layer, inference engine or processing layer, and user interface.
Core modules of a typical clinical decision support system
A data management layer combines
- a clinical database storing information on diseases, diagnoses, and lab findings;
- patient data; and
- a knowledge base in the form of if-then rules or machine learning models.
An inference engine or processing layer applies rules or algorithms and datasets from the knowledge base to available patient data. The results are displayed via a user interface layer — a mobile, web or desktop application, an EHR system dashboard or mobile text alerts.
Preserving the same structure, under the hood CDSSs vary in ways they come to a conclusion, falling into two types — knowledge-based and nonknowledge-based systems.
Knowledge-based CDSS
Systems of this type are built on top of a knowledge base in which every piece of data is structured in the form of if-then rules. For instance, if a new order for a blood test is placed and if the same blood test was made within the past 24 hours, then a duplication is possible.
The inference engine runs the built-in logic to combine the evidence-based rules with the patient’s medical history and data on his or her current condition. The results come in the form of alerts, reminders, diagnostic suggestions, a series of treatment options or ranked lists of possible solutions while the final word rests with a human expert.
Nonknowledge-based CDSS
The core difference from the previous group consists of applying machine learning models. Rather than consulting with a library of predefined if-then rules, such a system learns from past experiences and finds patterns in historical data. These are the two techniques most widely used in such CDSSs:
- genetic algorithms (GA) reflecting the mechanics of natural selection described by Charles Darwin. Just as species change from generation to generation to better fit their environment, GAs adapt to a new task, producing a number of random solutions and then iteratively evaluating and improving them until the most fitting option is found.
- artificial neural networks (ANN) that mimic human thinking. Similar to human brains, ANNs have a set of “neurons” called “neurods.” They are linked to each other with weighted connections that act as nerve synapses transmitting signals across the neural network.
Nonknowledge-based systems come with a promise to significantly cut healthcare costs and relieve the pressure on medical experts. However, there are issues preventing their large-scale adoption. They include a compute-intensive and time-consuming training process and the requirement of large datasets needed to improve accuracy of models. But the main obstacle is the lack of interpretability as systems can’t explain the reasoning behind generated decisions.
Due to drawbacks mentioned, modern CDSSs are primarily knowledge-based. Now, let’s see what decisions they are able to support.
CDSS major areas of application
Human brains are prone to error — especially, when dealing with large volumes of information in a high-stress hospital environment. Computerized systems can take a laboring oar of sifting through tons of data and making countless comparisons to narrow down the number of possible decisions — from hundreds and thousands to just a few .
Drug selection
Statistics show that 7,000 to 9,000 US patients die annually because of medication errors. Besides that, a lot more people suffer from complications caused by inappropriate medicines, ill-judged dosage, or drug incompatibility, increasing treatment costs by over 40 billion a year.
The good news is that nearly 50 percent of medication errors happen at the first — ordering or prescribing - stage. So, mistakes can be spotted and prevented before they cause any harm. And that’s where a decision support tool comes in handy, eliminating risks from human factors like distraction that accounts for around 75 percent of medication errors.
Using critical patient data such as weight, age, allergy status, and current prescriptions, CDSSs may automatically deal with the following tasks.
Drug allergy checking. The system matches an ordered medication against a patient’s list of documented allergies, evaluates the probability of unwanted reactions, and generates alerts.
Basic guidance on dosage. Dosing errors account for over 60 percent of all the prescribing mistakes. But this can be improved by a corresponding decision support module. In the simplest scenario, the software component generates a patient-specific list of recommended dosing parameters for a particular medication. It saves a clinician time on selection of the most appropriate dosage and frequency. The CDSS may as well alert experts to exceeding dosing limits.
Checking for duplicate therapy. A duplicate therapy occurs when two or more drugs with the same active ingredient are prescribed simultaneously. It leads to overdose and related adverse effects. The CDSS feature addressing this problem compares a newly added drug with active ingredients of drugs in a patient’s profile. If a match is detected, the system generates an alert.
Drug interactions checking. A drug's interaction with other substances may change its expected effect. Based on clinical documentation at hand, a CDSS considers interactions of a newly prescribed medication with
- other drugs in a patient’s list (drug-drug interactions or DDI),
- food and beverage (drug-food interactions),
- herbals,
- ethanol,
- testing (if the medication can affect the results of laboratory tests),
- pregnancy and lactation, and
- a patient’s disease that can also affect the drug’s performance (drug-disease interactions).
Today, many Computer Provider Order Entry (CPOE) systems come equipped with drug safety components that perform duplicate therapy, DDI and drug-dose checking. But you may find separate decision support modules to complete existing software as well. The example of a single-task solution is a drug allergy checker by PEPID which can be integrated with any EHR or other healthcare information system.
Diagnostic support
CDSSs for disease identification are called diagnostic decision support systems (DDSSs) or medical diagnosis systems (MDSs). They compare information on a patient's condition with a knowledge base and generate a list of possible diagnoses.
A specific example of a DDSS is a solution utilizing deep learning for diagnostic imaging. It would traditionally focus on a specific problem area — say, lung abnormalities or a particular type of cancer. Similar to other CDS tools, AI-fueled programs work as a second pair of eyes and make suggestions and alerts — rather than come to a final conclusion.
Cost containment
Integrated in a CPOE system, decision support tools may decrease treatment costs by suggesting cheaper drug alternatives or spotting test duplications. Studies revealed that CDSSs save hospital units hundreds of thousands of dollars per year by alerting to cases of excessive medical testing.
Clinical management
Some clinics employ decision support software to enhance adherence to clinical guidance. Similar to information about drugs and diseases, hospital rules can be encoded into a knowledge-based CDSS in the form of IF-THEN-ELSE pieces of information. Such solutions perform various tasks, from prompting nurses to take specific measurements according to a protocol to informing doctors about patients who don’t follow their treatment plans.
AUC for Medicare patients
AUC stands for appropriate use criteria that specify when exactly it makes sense to perform a certain medical service. Starting in January 2020, the Protecting Access to Medicare Act (PAMA) obliges American hospitals to comply with Medicare’s AUC program for advanced imaging like computer tomography (CT) or magnetic resonance imaging (MRI).
It means that prior to ordering an expensive test for a Medicare patient, a physician must consult a clinical decision support mechanism. Without a verdict made by a CDS tool ("appropriate," "may be appropriate," or "rarely appropriate,"), service providers won’t receive reimbursement for their procedures.
Now the program undergoes the so-called educational and testing period with no penalties charged while the full implementation is scheduled for 2021. At the end of the day, when all technological challenges are solved, the AUC initiative is expected to benefit both providers and patients by enhancing the quality of care and reducing expenses on tests.
No matter the primary declared reason for implementation, all CDSSs are built with a matter-of-course intention to cut healthcare costs while improving patient safety. The next part will describe the advances of existing systems in achieving this ambitious goal.
Key providers of clinical decision support software
Though there are multiple providers offering decision support modules for different tasks, the market is dominated by five major players — Siemens, Philips, IBM, Cerner Corporation, and Change Healthcare.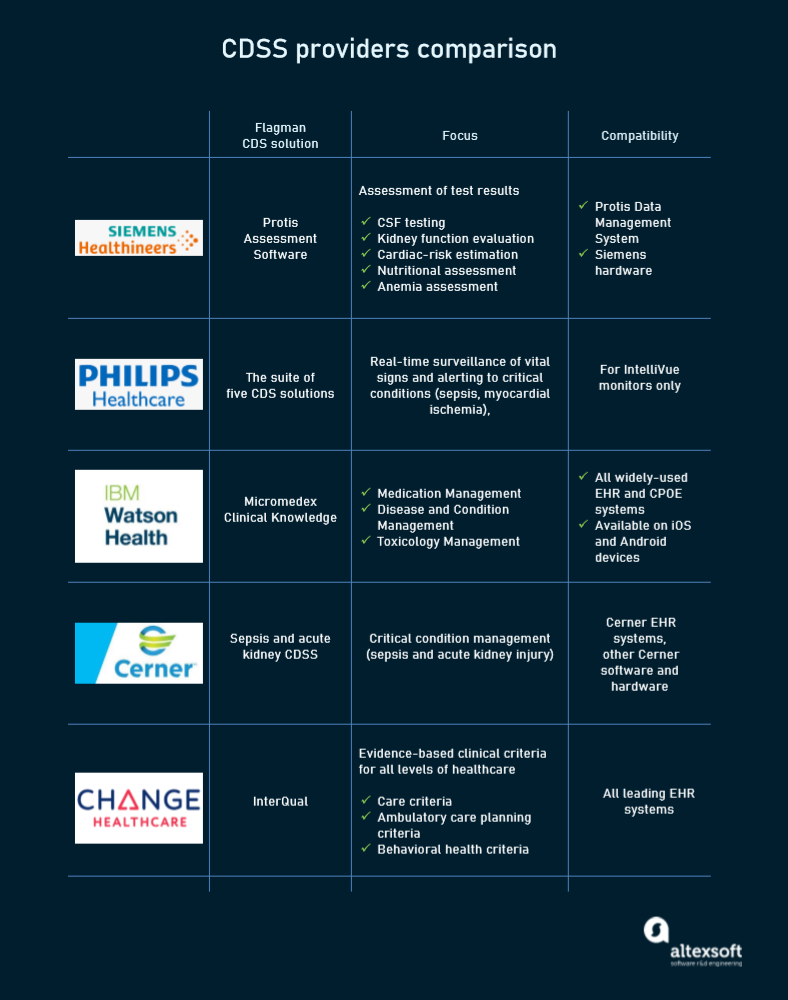
Offerings from leading CDSS vendors
Siemens Healthineers: strong focus on test results
A leading manufacturer of diagnostic imaging devices, Siemens Healthineers also offers a range of software solutions for healthcare centers. Its core decision support product is Protis Data Management System with Protis Assessment Software as an optional module. The former consolidates a patient’s test results from different platforms into a single graphical report. The latter helps physicians interpret clinical data.
Protis Assessment Software is a knowledge-based CDSS employing standard rules set by experts. It supports
- cerebrospinal fluid (CSF) testing used to diagnose conditions affecting the brain and spinal cord,
- evaluation of kidney function assisting with early detection of renal diseases,
- a 10-year cardiovascular risk estimation,
- an iron and anemia assessment, and
- nutritional assessment to recognize protein calorie malnutrition in inpatients. When not diagnosed and addressed, malnutrition increases the length of stay in the hospital and associated treatment costs.
The software provides easy-to-understand graphical reports and suggests interpretations and recommendations, thus saving time, reducing manual work, preventing unnecessary testing, and cutting treatment costs.
Besides Protis, the company offers the following CDS solutions:
- AI RAD Companion, an AI-powered cloud app to help with analyzing CT, X-ray and MRI scans of the brain, prostate, chest and other organs;
- Prisca system for prenatal risk calculation based on biochemical markers, ultrasound measurements, and demographics; and
- Medicalis, a cloud-based clinical decision support mechanism to ensure compliance with the AUC program.
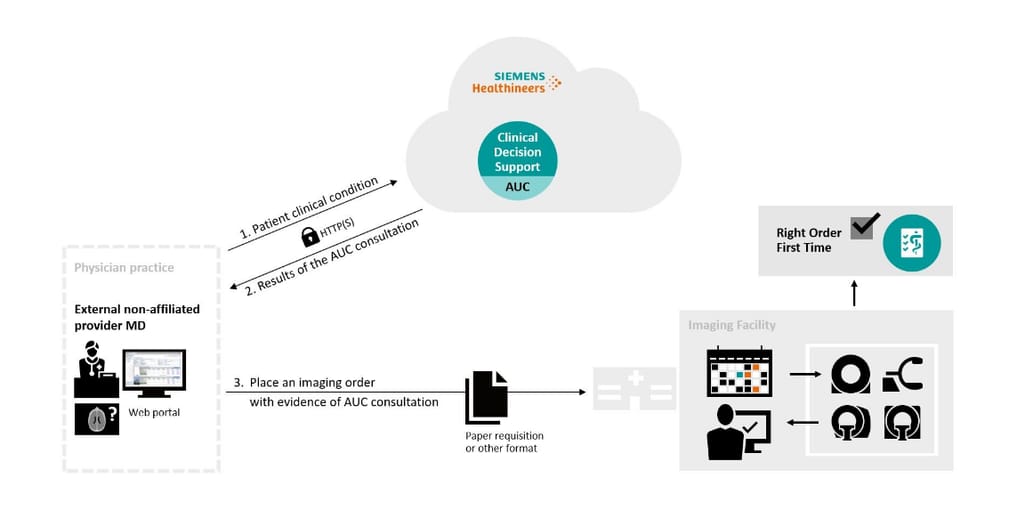
Medicalis CDS mechanism workflow
Philips Healthcare: continuous monitoring and sending alerts
Philips Healthcare division heavily invested in the development of CDSS solutions to complete the company’s patient monitoring systems. Currently, five tools are available for use with branded IntelliVue monitors by Philips.
Horizon Trends monitors vital signs (body temperature, pulse, breathing rate, and blood pressure) in real time and alerts to dangerous deviations.
ST Map focuses on the specific portion of ECG called ST-segment. Continuous ST-segment monitoring is recommended for patients with the acute coronary syndrome at risk of myocardial ischemia. ST Map allows medical staff to identify critical changes and make quick decisions.
Event Surveillance tracks up to four clinical parameters and notifies a physician when two, three, or four of them show critical deviations. The solution enables you to set specific thresholds and create “smart alarms” according to the needs of a particular patient. For example, you’ ll be notified if the heart rate changes by more than 50 percent within 60 seconds.
Monitoring of multiple parameters with IntelliVue. Source: MedicalExpo
ProtocolWatch Sepsis checks vital signs of a patient against sepsis criteria and notifies caregivers when these criteria are met.
The Histogram Trends module represents a patient’s measurements over an extended period of time. It allows a physician to see if a therapy or a particular medication has the desired effect.
IBM Watson Health: end-to-end management of drugs, diseases, and toxins
Micromedex Clinical Knowledge by IBM Watson Health is an evidence-based clinical decision support system used in over 4,500 hospitals worldwide. It integrates with all widely-used EMR and CPOE systems. The modular structure allows hospitals to add functionality gradually, as and when necessary. Currently, Micromedex contains three large components.
A Medication Management module provides complete information on drugs and checks all types of drug interactions including drug-drug, drug-disease, drug-food, drug-laboratory, drug-ethanol, drug-pregnancy, and drug-lactation, pinpointing potentially dangerous or unwanted combinations.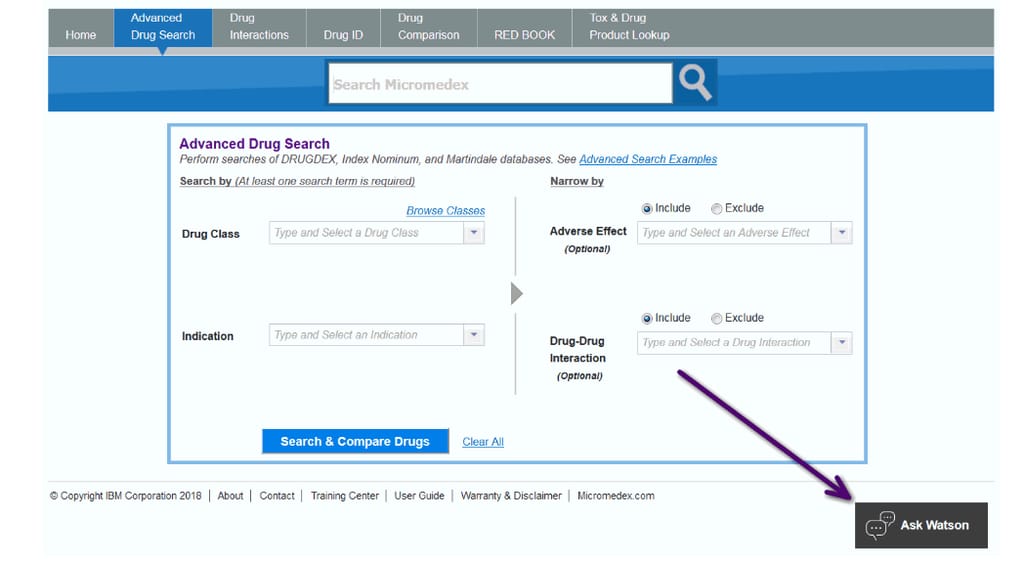
Micromedex Medication Management interface with a built-in Watson Assistant chatbot. Source: Micromedex Solutions
It also features a drug dosage calculator and makes suggestions on herbal and other alternative therapies that can be used alongside conventional medicine.
A Disease and Condition Management module ensures quick access to treatment information, minimizing errors, cutting treatment costs and preventing unnecessary exams and procedures.
A Toxicology Management module is used across all American certified Poison Control Centers and emergency departments to identify potential poison sources, provide toxicology analysis, and make quick informed decisions in case of chemical spills and exposures.
In March 2020, IBM announced a partnership with DynaMed, a clinical reference resource providing quick answers to medical questions across many specialties. The two companies offer a combined DynaMed and Micromedex with Watson platform for clinicians at the point of care. At the same time, they continue to sell their own solutions separately.
Cerner: addressing critical conditions
Cerner is a global provider of health information technologies. Besides end-to-end EHR systems and numerous clinical software tools, the company delivers connectivity hardware components and medical devices. Its suite of CDS tools is designed for most critical conditions when every hour is crucial.
A sepsis CDSS aims at early recognition of life-threatening infection in the bloodstream. The system was built after Cerner co-founder Neal Patterson lost his sister-in-law to sepsis triggered by pneumonia. She didn’t get timely treatment as doctors failed to recognize early signs of the disease. By now, Cerner sepsis surveillance solution is implemented in hundreds of hospitals across the USA. It continuously looks to a patient’s vital signs, and when spotting patterns typical to sepsis, alerts a clinical team.
An acute kidney injury (AKI) solution addresses another dangerous condition that requires early detection and prompt treatment. The module looks for changes in serum creatinine levels in urine. Once its concentration shows a dangerous rise the system notifies clinicians and makes suggestions on what to do next.
A Rapid Response component integrates with sepsis and AKI modules to enable immediate intervention when vital signs start changing rapidly and unexpectedly.
Change Healthcare: strict adherence to criteria at all levels of care
Change Healthcare, one of the largest tech providers in the medical field, offers solutions connecting hospitals, patients, and payers. The company’s networks manage one-third of all clinical records across the USA. Its clinical decision support solution called InterQual boasts a 40-year history of accumulating knowledge. The system provides access to evidence-based criteria — or nationally recognized standards of appropriate care — divided into several large groups.
Level of Care Criteria help clinicians recognize symptoms, evaluate the severity of a patient’s condition and effectiveness of treatment. It recommends the next steps in case of complications or slow response to therapy.
Ambulatory Care Planning Criteria suggest when tests, consultations, and medications are valid so that hospitals may avoid excessive exams and procedures.
Behavioral Health Criteria focus on the needs of patients with psychiatric and substance abuse disorders. The module assists caregivers with choosing the appropriate therapy based on current functional status.
Change Healthcare is constantly updating its content with the latest evidence. It employs a surveillance system that automatically analyzes over 3,000 medical sources daily and chooses newly published information to be reviewed by the expert team. The 2020 InterQual version comes with hundreds of enhancements including care guidance for COVID-19 patients.
The flagman system can be completed with a couple of useful cloud-based tools.
InterQual AutoReview is the first healthcare solution automating the medical review process. It uses Natural Language Processing (NLP) models to pull data from the EHR and identify diagnostic information in unstructured clinical content.
CareSelect Imaging brings advanced imaging guidelines into existing EHR workflows to meet PAMA requirements.
How to settle on a decision support system: challenges and possible drawbacks
CDS systems contribute to better healthcare, but they are not without their own risks and drawbacks. To understand which decision support solution will bring the most value to a particular medical center, it’s necessary to consider challenges adopters of the technology typically face.
Alert fatigue. A CDSS may generate too many alerts and recommendations. As a result, caregivers start ignoring them regardless of importance. Make sure that the solution you opt for has a mechanism to select and prioritize critical notifications.
Integration issues. All required functionality in place, a CDS solution won’t yield much benefit if not teamed up with the existing information system. You need to check if the solution is compatible with the EHR or can be relatively easily integrated into the workflow.
Lack of interoperability. Even upon incorporation into the hospital IT ecosystem, clinical decision solutions can fail to effectively communicate with other modules due to the diversity of healthcare record standards. Fortunately, the situation is constantly changing for the better with wider adoption of Fast Healthcare Interoperability Resources (FHIR), the latest HL7 format for exchanging and sharing healthcare information. It is already utilized by many EHR providers and medical organizations. To guarantee smooth data exchange, the standard should be adopted at all levels of a healthcare organization and by external systems you are going to use.
Cost of adoption. Implementation of the end-to-end CDSS entails significant investments. Customization and integration with the current infrastructure will by far increase the total cost of adoption. If you are on a tight budget, consider solutions with modular structure and flexible settings so that you can build your system step by step and tailor it to your requirements.

